Washington Post’s Katherine Ellison on the striking decrease in mortality from lung and breast cancer in the US:
There are many and varied explanations for the progress, says Memorial Sloan Kettering oncologist Larry Norton, including “better early diagnosis, better imaging, better blood tests, better preventive measures and better treatments, including precision medicine with gene-profiling of patients’ tumors.”
The rest of the article focuses on treatments — immunotherapy in particular — [Note: And yes, of course dostarlimab was mentioned. Once a darling, always a darling. ] and cancer survivorship, but in discussing decreasing deaths from lung and breast cancer the article missed an opportunity for some education in cancer epidemiology.
The two sources chosen to present these data, ASCO’s cancer.net for lung and Breastcancer.org for breast are lacking in two ways: they are an impenetrable wall of text without much context, and they both have an agenda. Now, it happens that I agree with ASCO’s agenda — I am a dues-paying member — and don’t know enough Breastcancer.org to form an opinion, but neutral parties they are not. If only there was a tax-funded, publicly available database which could help us visualize trends in cancer statistics.
Now it so happens that the CDC maintains such a database, with its very on visualization tools, and it is exactly what we need. It will even make your PowerPoint slides for you! And yes, deaths from both lung and breast cancer have been steadily decreasing for the past two decades.
Lung and female breast cancer mortality in the United States, 1999–2020.
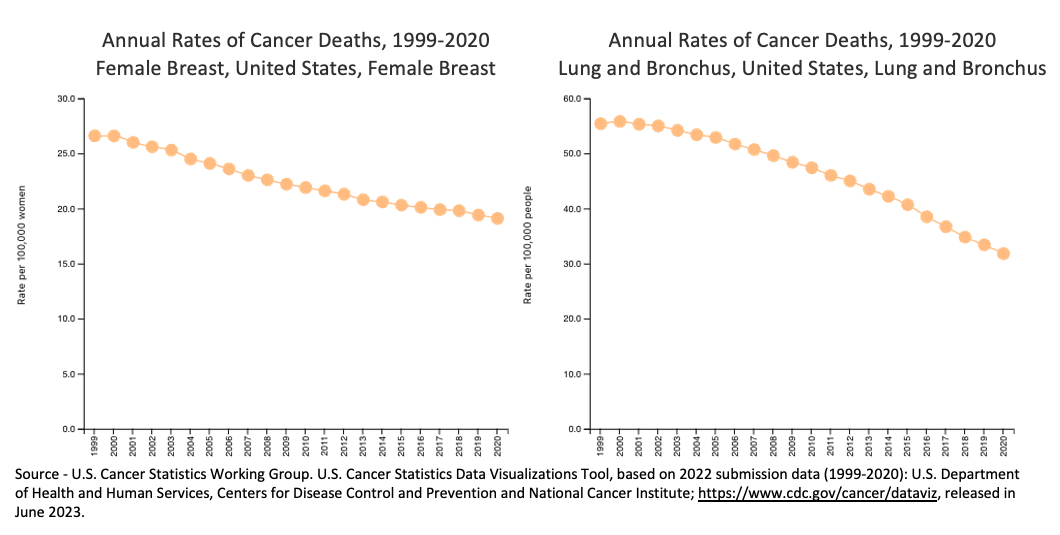
But is it because of better prevention, early diagnosis, more effective treatments, or all three? Looking at cancer incidence — the number of newly diagnosed cases per year — may help some. Better prevention would lead to decreased incidence, early detection would lead to an increase, a combination of the two may cancel each other out leading to a flat line, and any change in treatments would not affect it at all.
Lung and female breast cancer incidence in the United States, 1999–2020.
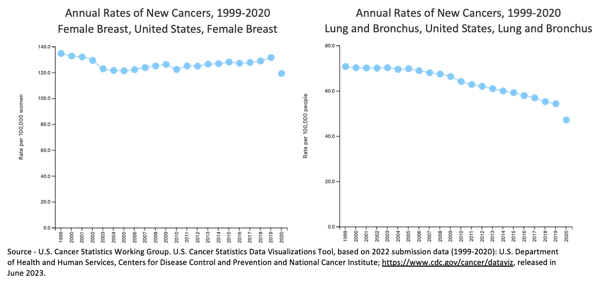
A slight initial dip in female breast cancer incidence followed by an even slighter increase make me think that early detection — all those mammograms — is superimposed on better prevention. The case is less ambiguous for lung cancer: the incidence is plummeting. In both cases, “prevention” was initiated by the 1964 Surgeon General’s report on tobacco smoke which led to massive anti-smoking campaigns from the 1970s onwards. The results weren’t immediately obvious — not having to air out all your clothes after a night out notwithstanding — but cancer rates started dropping after 20 years, and 50 years later we are reaping the full benefits.
Note that in lung cancer the mortality slope is steeper than the incidence slope. And while this may be explained by early detection and better treatments, it is possible that at least some of the improvement over newly diagnosed lung cancers is due to non-smoking associated lung cancer being generally less aggressive and occurring in younger and healthier people than tobacco-associated cancers. What could help unravel these different components — and highlight the increasing importance of cancer survivor healthcare — would be a prevalence curve: how many people in the United States are currently living with a particular cancer. Alas, those data are not available.
If you thought interpreting those four curves was interesting, do go back to the CDC database and check out the incidence and mortality curves for thyroid cancer — that poster child of over-diagnosis — and prostate cancer, the incidence of which fluctuates ever which way with changing screening recommendations but with mortality marching downwards for the last 20 years.